 The morphology of the P wave will not be similar to the sinus P wave, which is normally upright in lead II and biphasic in lead V1. When faster, it is referred to as an accelerated junctional rhythm.īecause the electrical activation originates at or near the AV node, the P wave is frequently not seen it can be buried within the QRS complex, slightly before the QRS complex or slightly after the QRS complex. A junctional rhythm is normally slow - less than 60 beats per minute. Can cause cardiomyopathy.A junctional rhythm occurs when the electrical activation of the heart originates near or within the atrioventricular node, rather than from the sinoatrial node.īecause the normal ventricular conduction system (His-Purkinje) is used, the QRS complex is frequently narrow. May not respond to DC cardioversion or adenosine. Neonates (then not again until adulthood) Saw tooth flutter waves (often only appreciated with AV block from adenosine)įixed but may appear irregular depending on AV conduction Up to 500 beats/min in neonates (300 beats/min in children) with variable AV conduction being common Neonates and infants (220 (commonly 250-300 in infants) If unsuccessful, or child deteriorates, proceed to medical treatment as per the algorithmĭO NOT perform Eyeball pressure or carotid sinus massage as they are no longer recommended.Continuous cardiac monitoring should be applied prior to performing.Vagal manoeuvres are safe, minimally invasive and effective for reverting SVT in a hemodynamically stable child or infant.*Adapted from the Sydney Children’s Hospital Network Guideline on SVT 1. Blood tests provide no added benefit to the diagnosis or management and therefore are not recommended, unless considering other causes of SVT.CXR can be considered if clinical signs of heart failure present.(See additional notes below for further details) Are P-waves present and what is their morphology?.Is there a broad or narrow QRS complex?. 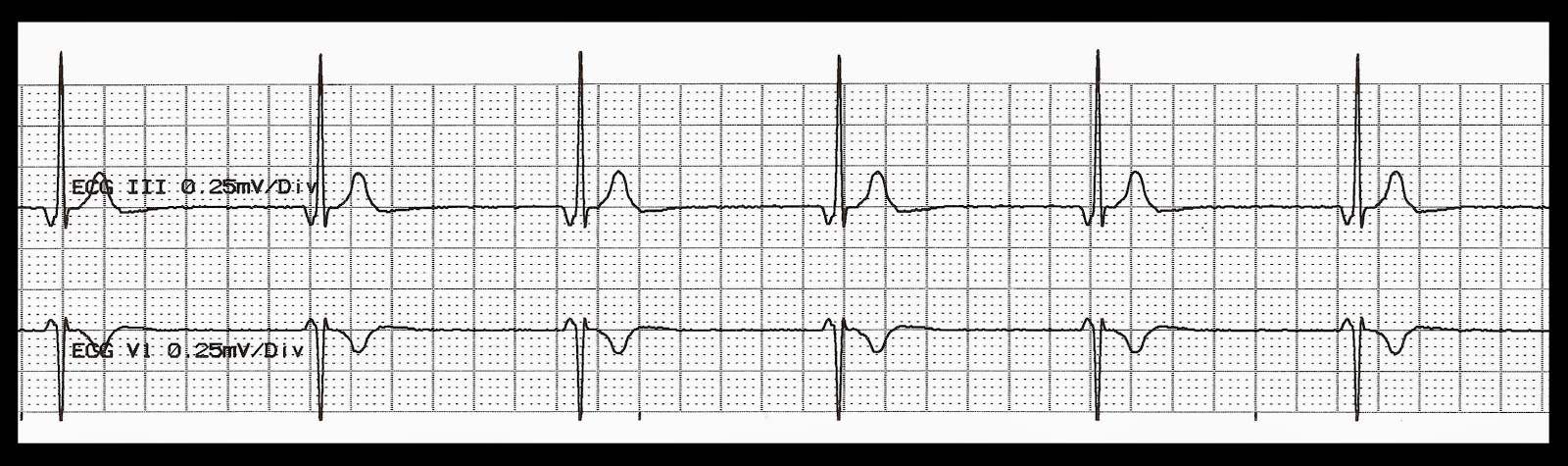
Red Flags Unwell appearance, hypotension, drowsiness/altered conscious state Note: BP machines and pulse oximeters may be unreliable at common SVT ratesġ2 lead ECG (pre and post reversion techniques) Typically present late, with signs of congestive heart failure (respiratory distress, hepatomegaly, oedema) Irritability, poor feeding, lethargy and sweatingĬhild complains of feeling ill, breathless, chest pain, nausea, dizziness or sweating Tolerate tachycardia well, making early signs and symptoms initially subtleĪble to perceive palpitations and therefore present earlier with less clinical signs or symptoms The priority is to identify the child in shock (pallor, poor perfusion, decreased consciousness, hypotension) and proceed immediately to resuscitation (see flowchart below) Factors that may contribute to tachycardia (eg sepsis, pain, dehydration, anxiety, and fever) should also be considered and addressed when managing a patient presenting with a tachyarrhythmia. 
Always assume a broad complex tachycardia is due to VT rather than SVT with aberrancy, unless there is clear evidence it is not VT.Onset and offset are abrupt, and p-waves are either not visible or seen after the QRS complexes (See additional notes below for important features when differentiating between different causes of narrow complex tachyarrhythmias) SVT typically has a fixed rate, usually >220 bpm. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
